Question: I don’t play tennis; how can I have tennis elbow?
Answer: Easily, lateral epicondylitis, a.k.a. tennis elbow has little to do with tennis and lots to do with constantly using your arm in a repetitive motion.
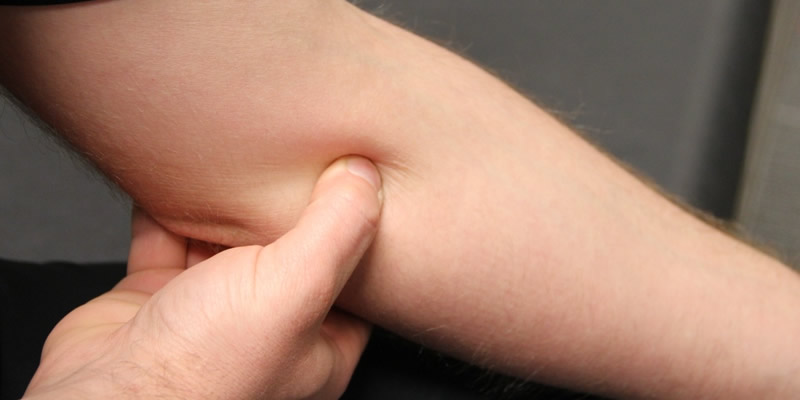
Epicondyles are the bony bumps on the inside and outside of your elbow. Epicondylitis is the inflammation of these. 95% of people suffering from this do not play tennis, but this is a common sports related injury. This can be a result of any sport where your arm is in a similar position or even work related such as carpentry, plumbing or constant use of a computer keyboard. Even musicians are vulnerable!
After repeated use, the tendons at the elbow end of the extensor carpi radialis brevis (ECRB) muscle may develop small tears. This leads to inflammation and stress on the rest of your arm. It is a form of tendonitis. This can be a result of any activity that requires repetitive arm, wrist, or elbow movement. The extensor tendons are used when extending your wrist and fingers. The flexor tendons are needed for closing wrist and fingers. Both flexor and extensors are used in thousands of tasks, and often handle very high levels of stress.
Inflammation is a normal part of the healing process and the body’s natural response to an immediate injury. Swelling, discomfort, the sensation of heat, redness, and loss of function are the key symptoms which should warn you something is not right in your world. Tenderness and stiffness are also red flags, and when the pain is severe enough, it may radiate down the arm, into the hand and fingers.
Approximately 3% of the population experiences this injury, typically occurring in men and women between the ages of 40 and 50. Your daily activity is a big determining factor in your likeliness to be affected. Office workers, secretaries and Health Care Workers are especially prone.
Self-diagnosis is a dangerous thing as there may be more than one potential issue with the same symptoms.
As with any injury or ailment, the first step is to visit your physician. Dr. Marshall Allegra spends quality time speaking with each patient at his Hazlet office to understand their unique condition based on symptoms and life-style. He has over 25 years’ experience diagnosing pain and prescribing the most appropriate treatment, exploring all non-surgical possibilities first. Common remedies and treatments Dr. Allegra may suggest:
- Cold therapy treatments should be in the earliest stages of an injury only as this will actually impede the recovery because cold restricts the vessels – reducing the blood flow to the area
- Anti-inflammatory medication may relieve the pain
- Limit activities for a few days or possibly weeks until the inflammation subsides. If possible, avoid the repetitive movement.
- A brace may help stabilize the area and limit movement for you
- Supervised strengthening and stretching exercises may help, but be sure to do the correct ones in the correct position or you may further injure yourself. A physical therapist can work out a routine for you to safely improve your symptoms.
- Acupuncture
- Steroid injections directly into the inflamed area target the inflammation.
- Surgery when all else fails.
It is essential to allow all injuries to heal completely before returning to your daily activities. You want to avoid the build-up of scar tissues or having on-going issues. Be sure to follow up with Dr. Allegra before returning to your routine.
Contact Dr. Marshall P. Allegra
879 Poole Avenue, Hazlet New Jersey, 07730
Phone: (732) 888-8388





 Shoulder Anatomy
Shoulder Anatomy