Walking is a great way to improve or maintain your overall health. Just 30 minutes every day can increase cardiovascular fitness, strengthen bones, reduce excess body fat, and boost muscle power and endurance. It can reduce your risk of developing conditions like heart disease, type 2 diabetes, osteoporosis and some cancers. Unlike some other forms of exercise, walking is free and doesn’t require any special equipment or training.
Physical activity does not have to be vigorous or done for long periods in order to improve your health. Even a low level of exercise – around 75 minutes per week – improves fitness levels significantly, when compared to a non-exercising group.
Walking is low impact, requires minimal equipment, can be done at any time of day and can be performed at your own pace. You can get out and walk without worrying about the risks associated with some more vigorous forms of exercise. It’s also a great form of physical activity for people who are overweight, elderly, or who haven’t exercised in a long time.
Health benefits of walking
You carry your own body weight when you walk. This is known as weight-bearing exercise. Some of the benefits include:
- Increased cardiovascular and pulmonary (heart and lung) fitness
- Reduced risk of heart disease and stroke
- Improved management of conditions such as hypertension (high blood pressure), high cholesterol, joint and muscular pain or stiffness, and diabetes
- Stronger bones and improved balance
- Increased muscle strength and endurance
- Reduced body fat
Walking for 30 minutes a day
To get the health benefits, try to walk for at least 30 minutes as briskly as you can on most days of the week. ‘Brisk’ means that you can still talk but not sing, and you may be puffing slightly. Moderate activities such as walking pose little health risk but, if you have a medical condition, check with your doctor before starting any new exercise program of physical activity.
Building physical activity into your life
If it’s too difficult to walk for 30 minutes at one time, do regular small bouts (10 minutes) three times per day and gradually build up to longer sessions. However, if your goal is to lose weight, you will need to do physical activity for longer than 30 minutes each day. You can still achieve this by starting with smaller bouts of activity throughout the day and increasing these as your fitness improves.
Physical activity built into a daily lifestyle plan is also one of the most effective ways to assist with weight loss and keep weight off once it’s lost.
Some suggestions to build walking into your daily routine include:
- Take the stairs instead of the elevator (for at least part of the way)
- Get off the bus one stop earlier and walk to work or home
- Do housework, like vacuuming
- Walk (don’t drive) to local stores
- Walk the dog (or your neighbor’s dog)
Wearing a pedometer while walking
A pedometer measures the number of steps you take. You can use it to measure your movement throughout a day and compare it to other days or to recommended amounts. This may motivate you to move more. The recommended number of steps accumulated per day to achieve health benefits is 10,000 steps or more.
Warming up and cooling down after walking
The best way to warm up is to walk slowly. Start off each walk at a leisurely pace to give your muscles time to warm up, and then pick up the speed. Afterwards, gently stretch your leg muscles – particularly your calves and front and back thighs. Stretches should be held for about 20 seconds. If you feel any pain, ease off the stretch. Don’t bounce or jolt, or you could overstretch muscle tissue and cause microscopic tears, which lead to muscle stiffness and tenderness.
It’s best to dress lightly when you do physical activity. Dressing too warmly can increase sweating and build up body temperature, which can make you uncomfortable during a walk or possibly cause skin irritations. A gradual cool-down will also prevent muscular stiffness and injury.
Footwear for walking
Walking is a low-cost and effective form of exercise. However, the wrong type of shoe or walking action can cause foot or shin pain, blisters and injuries to soft tissue. Make sure your shoes are comfortable, with appropriate heel and arch supports. Take light, easy steps and make sure your heel touches down before your toes. Whenever possible, walk on grass rather than concrete to help absorb the impact.
Safety suggestions while walking
Walking is generally a safe way to exercise, but look out for unexpected hazards. Suggestions include:
- See your doctor for a medical check-up before starting a new fitness program, particularly if you are aged over 40 years, are overweight, or haven’t exercised in a long time.
- Pre-exercise screening can identify medical conditions that may put you at a higher risk of experiencing a health problem during physical activity. It is a filter or safety net to help decide if the potential benefits of exercise outweigh the risks for you.
- Visit an orthopedic physician if you develop any pain that doesn’t go away in just a few days.
- Choose walks that suit your age and fitness level. Warm up and cool down with a slow, gentle walk to ease in and out of your exercise session.
- Wear loose, comfortable clothing, and appropriate footwear to avoid blisters and shin splints.
- Wear sunglasses, sunscreen, long sleeves and a hat to avoid sunburn.
- Take waterproof clothing to avoid getting wet if it rains.
- Drink plenty of fluids before and after your walk. If you are taking a long walk, take water with you.









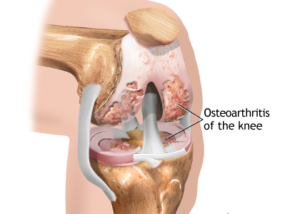 Patients with unicompartmental knee arthritis have cartilage degeneration in only one section or compartment of the knee. In cases where nonsurgical techniques do not provide sufficient symptom relief, surgeons can remove damaged cartilage and bone in the diseased area only, while preserving the ligaments that help support the knee joint.
Patients with unicompartmental knee arthritis have cartilage degeneration in only one section or compartment of the knee. In cases where nonsurgical techniques do not provide sufficient symptom relief, surgeons can remove damaged cartilage and bone in the diseased area only, while preserving the ligaments that help support the knee joint.
 Shoulder Anatomy
Shoulder Anatomy