For young athletes, sports activities are more than just play.
Participation can improve physical fitness, coordination, and self-discipline, and help children learn teamwork.
However, children’s bones, muscles, tendons, and ligaments are still growing, making them more susceptible to injury. Growth plates are the areas of developing cartilage at the ends of long bones where bone growth occurs in children. The growth plates are weaker than the nearby ligaments and tendons. A twisted ankle that might result in a sprain in an adult, could result in a more serious growth plate fracture in a young athlete.
There are also significant differences in coordination, strength, and stamina from child to child and between children and adults. Young athletes of the same age can differ greatly in size and physical maturity. Grade school students are less likely to experience severe injuries during athletic activities because they are smaller and slower than older athletes. High school athletes, however, are bigger, faster, stronger, and capable of delivering tremendous forces in contact sports.
Acute sports injuries are caused by a sudden trauma, such as a twist, fall, or collision. Common acute injuries include broken bones, sprains (ligament injuries), strains (muscle and tendon injuries), and cuts or bruises.
Most acute injuries should be evaluated by an orthopedic physician. Prompt first aid treatment should be provided by coaches and parents when the injury occurs. This usually consists of the RICE method: rest, applying ice, wrapping with elastic bandages (compression), and elevating the injured arm, hand, leg, or foot. This usually limits discomfort and reduces healing time. Proper first aid will minimize swelling and help the doctor establish an accurate diagnosis.
Follow these tips to play it safe:
• Always be in proper physical condition to play a sport
• Know and abide by the rules of a sport
• Wear appropriate protective gear
• Know how to correctly use athletic equipment
• Always warm up before playing
• Stay hydrated
• Avoid playing when very tired or in pain
Following a regular conditioning program with exercises designed specifically for their chosen sport can help young athletes avoid injuries.
Coaches and parents are responsible for creating an atmosphere that promotes teamwork and sportsmanship. A young athlete striving to meet the unrealistic expectations of others may ignore warning signs of injury and continue to play with pain. The “win at all costs” attitude of many parents, coaches, professional athletes and peers can lead to injuries. Above all else, youth sports should always be fun.



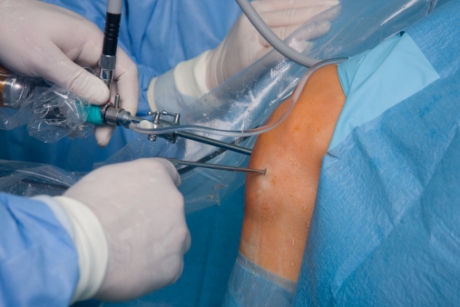



 Microfracture surgery has gained popularity in sports in recent years; numerous professional athletes including members of the NBA (most notably Andrew Bogut, Anfernee Hardaway, Jason Kidd, Greg Oden, Allan Houston, Kenyon Martin, Tracy McGrady, Chris Webber and Amar’e Stoudemire, MLB (Jeff Clement), Matt Kemp, Derek Holland, NFL and NHL players have undergone the procedure.
Microfracture surgery has gained popularity in sports in recent years; numerous professional athletes including members of the NBA (most notably Andrew Bogut, Anfernee Hardaway, Jason Kidd, Greg Oden, Allan Houston, Kenyon Martin, Tracy McGrady, Chris Webber and Amar’e Stoudemire, MLB (Jeff Clement), Matt Kemp, Derek Holland, NFL and NHL players have undergone the procedure.