You’re working at your desk, trying to ignore the tingling or numbness you’ve had for months in your hand and wrist. Suddenly, a sharp, piercing pain shoots through the wrist and up your arm. Just a passing cramp? More likely you have carpal tunnel syndrome, a painful progressive condition caused by compression of a key nerve in the wrist.
Carpal tunnel syndrome occurs when the median nerve, which runs from the forearm into the palm of the hand, becomes pressed or squeezed at the wrist. The median nerve controls sensations to the palm side of the thumb and fingers as well as impulses to some small muscles in the hand that allow the fingers and thumb to move. The carpal tunnel – a narrow, rigid passageway of ligament and bones at the base of the hand – houses the median nerve and tendons.
Women are three times more likely than men to develop carpal tunnel syndrome, perhaps because the carpal tunnel itself may be smaller in women than in men. The dominant hand is usually affected first and produces the most severe pain. Persons with diabetes or other metabolic disorders that affect the body’s nerves and make them more susceptible to compression are also at high risk.
Early diagnosis and treatment by an orthopedic doctor are important to avoid permanent damage to the median nerve. Treatments for carpal tunnel syndrome should begin as early as possible, under a doctor’s direction. Underlying causes such as diabetes or arthritis should be treated first. Initial treatment generally involves resting the affected hand and wrist for at least 2 weeks, avoiding activities that may worsen symptoms, and immobilizing the wrist in a splint to avoid further damage from twisting or bending. If there is inflammation, applying cool packs can help reduce swelling.
Nonsteroidal anti-inflammatory drugs may ease symptoms. Other medications can be injected directly into the wrist or taken orally to relieve pressure on the median nerve, providing immediate, temporary relief.
Stretching and strengthening exercises supervised by a physical therapist, who is trained to use exercises to treat physical impairments, or an occupational therapist, who is trained in evaluating people with physical impairments and helping them build skills to improve their health and well-being, may be ordered by your orthopedic physician.
Alternative therapies such as acupuncture and yoga have been shown to reduce pain and improve grip strength among patients with carpal tunnel syndrome.
Carpal tunnel release is one of the most common surgical procedures in the U.S. Generally recommended if symptoms last for 6 months, surgery involves releasing the ligament around a portion of the wrist that compresses the median nerve. Surgery is done under local anesthesia and does not require an overnight hospital stay.
Although symptoms may be relieved immediately after surgery, full recovery from carpal tunnel surgery can take several months. Patients should undergo physical therapy after surgery to restore wrist strength.
Recurrence of carpal tunnel syndrome following treatment is rare. The majority of patients recover completely.
You can help to prevent this disabling occupational illness by performing stretching exercises, taking frequent rest breaks, wearing splints to keep wrists straight, and by being mindful to maintain correct posture and wrist position.







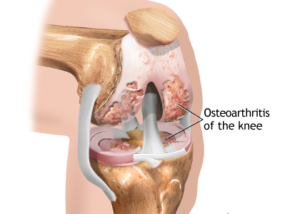 Patients with unicompartmental knee arthritis have cartilage degeneration in only one section or compartment of the knee. In cases where nonsurgical techniques do not provide sufficient symptom relief, surgeons can remove damaged cartilage and bone in the diseased area only, while preserving the ligaments that help support the knee joint.
Patients with unicompartmental knee arthritis have cartilage degeneration in only one section or compartment of the knee. In cases where nonsurgical techniques do not provide sufficient symptom relief, surgeons can remove damaged cartilage and bone in the diseased area only, while preserving the ligaments that help support the knee joint.
 Shoulder Anatomy
Shoulder Anatomy