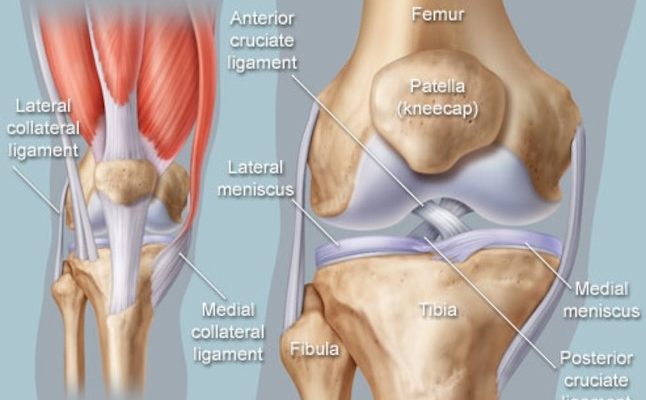
Why do so many people have problems with their knees? Possibly because the knee is one of the largest and most complex joints in the body?
The knee joins the femur (thigh bone) to the Tibia (shin bone). A smaller bone runs alongside the tibia called the fibula, and the kneecap, or patella, are the other bones that make the knee joint. The kneecap rests against a groove at the end of the femur, allowing it to move around.
Additionally, all of these bones have a protective layer of tissue called cartilage which provides cushioning, allowing the bones to glide around without difficulty. Between the femur and tibia are disks of tissue called menisci which also help absorb the pounding the knee takes. Now add tendons (which connect the knee bones to the leg muscles that move the knee joint) and ligaments (which join the knee bones and provide stability to the knee). Your knee also contains many bursae, or fluid-filled sacs, help the knee move smoothly.
That is a lot of moving parts and soft tissue in a body part that takes a lot of abuse. People seem to only realize how much they depend on their knees when they experience pain during movement.
Some of the most common knee injuries/issues are:
Dislocations when the bones of the knee get out of place. This can happen during a fall or impact, especially involving twisting.
Fractures of the patella or kneecap are common from a sports injury or a fall. Your kneecap is your first line of defense as it protects the knee joint.
Anterior Cruciate Ligament (ACL) Injuries effects the ligament that joins the lower and upper leg bones together, which stabilizes the knee. They account for around 40% of sports injuries.
Posterior Cruciate Ligament (PCL) Injuries involve the ligament which connects the shinbone and the femur. It’s located at the back of your knee and aids in preventing the shinbone from moving too far backwards.
Meniscal Tears are a damage to the piece of cartilage which acts like a cushion between the femur and tibia bones.
Tendon Tears of the quadriceps and patellar tendons are more common in middle age.
Osteoarthritis makes the protective cartilage grow thin and rough, which leaves the bones in the joint with less protection. Walking becomes painful when the bones can become damaged.
Tendonitis involves inflammation of a tendon. Tendons can also be torn.
Bursitis, or pain, swelling, and warmth in any of the bursae of the knee.
Rheumatoid Arthritis is an autoimmune condition that can cause arthritis in any joint, including the knees.
If you feel you have injured your knee, try RICE Therapy as soon as possible.
Rest (or reducing daily activities)
Ice
Compression (as with bandage support)
Elevation
Seeking medical treatment quickly can reduce the injury and the healing time.
A Physical Examination by a doctor gathers information about potential causes of damage or strain on the knee. Your orthopedist can perform a variety of tests to determine the problem, and the possible solutions, to take you out of pain and back into your normal lifestyle.
Once your injury is diagnosed, there are many options your doctor will go over. They will usually begin with the least invasive.
- Over-The-Counter pain medication to alleviate your pain while healing occurs.
- Physical therapy can strengthen the muscles surrounding the knee, increasing the knee’s stability using an exercise plan made by a trained PT.
- Cortisone Injection of a steroid into the knee may help reduce pain and swelling.
- Hyaluronan Injection into the knee may reduce pain from arthritis and delay the need for knee surgery in some people.
- Knee Surgery may be needed to correct a variety of knee conditions such as replacing or repairing a torn ligament, remove an injured meniscus, or entirely replace a severely damaged knee.
Dr. Marshall Allegra spends time speaking with each patient at his office in Hazlet to understand their unique condition. With over 25 years of experience as an orthopedic surgeon, Dr. Allegra is an expert at diagnosing pain and prescribing the most appropriate non-surgical interventions before surgery is recommended.